An ACL tear, often referred to as a torn ACL, can feel like a devastating blow—especially if you’re an active person who loves running, hiking, playing weekend basketball, or simply chasing your kids around the yard. The traditional advice has long been straightforward: surgery, followed by months of grueling rehabilitation.
But what if there’s another path?
Advances in regenerative medicine are changing how we think about treating anterior cruciate ligament tears. Stem cell therapy is emerging as a promising option for certain patients who want to avoid the operating room and get back to their lives faster.
In this guide, we’ll break down everything you need to know about using stem cells to treat an ACL tear—what works, what doesn’t, and how to find out if you’re a good candidate.
Fast Answer: Can Stem Cells Help an ACL Tear?
Yes, stem cell therapy may help certain ACL tears heal without surgery. Research shows that stem cell injections can reduce inflammation, promote new collagen production, and support the natural healing process in the injured ligament. For carefully selected patients—particularly those with partial ACL tears—this approach can mean less pain, faster recovery, and potentially avoiding reconstruction surgery altogether.
At Stem Cells LA (the regenerative medicine arm of Best Hair Transplant in Los Angeles/Redondo Beach), we use autologous stem cells derived from your own bone marrow combined with platelet rich plasma to support ACL healing. This cell therapy approach harnesses your body’s natural repair mechanisms rather than replacing the ligament with a graft.
Here’s what you need to know upfront:
-
Stem cell treatment works best for partial ACL tears or acute injuries where the ligament is still connected
-
It’s not a guaranteed replacement for anterior cruciate ligament reconstruction in every patient
-
Complete tears with significant laxity may still require surgical treatment
Recovery comparison:
|
Treatment |
Typical Recovery Timeline |
|---|---|
|
ACL reconstruction surgery |
9–12+ months before return to sports |
|
Stem cell therapy (appropriate candidates) |
Light activity in weeks; progressive sports return in 2–3 months |
Ready to find out if stem cell therapy could work for your ACL injury?
📞 Call Stem Cells LA today for a free consultation or fill out our online form. We serve patients throughout Los Angeles, Redondo Beach, Torrance, Manhattan Beach, and the greater South Bay area.
Understanding ACL Tears and Their Effects
The anterior cruciate ligament (ACL) is one of four major ligaments that stabilize your knee joint. Running diagonally through the center of your knee, this band of ligament tissue prevents your shin bone (tibia) from sliding forward and controls rotational movements when you pivot or change direction.
When you experience a torn ACL, the consequences extend far beyond immediate pain.
How ACL Tears Happen
Most ACL injuries occur during activities that stress the knee’s rotational stability:
-
Sudden pivots while your foot stays planted (common in soccer and basketball)
-
Awkward landings from jumps
-
Rapid deceleration when stopping quickly
-
Non-contact twisting motions (surprisingly, most ACL tears don’t involve collision)
-
Direct impact to the knee during football or skiing

Recognizing an ACL Tear
If you’ve torn your ACL, you likely experienced some of these symptoms:
-
A distinct “pop” sound or sensation at the moment of injury
-
Immediate swelling within the first few hours
-
Sharp knee pain that makes weight-bearing difficult
-
A feeling that your knee might “give out” or buckle
-
Difficulty walking, especially on uneven surfaces or stairs
The Long-Term Impact of an Untreated ACL
Here’s what many people don’t realize: the anterior cruciate ligament has a poor healing capacity on its own. Unlike muscles or skin, this ligament tissue lacks significant blood supply, which limits natural repair.
Without proper treatment, an injured ACL can lead to:
-
Chronic instability that limits everyday activities
-
Secondary meniscal tears from abnormal knee mechanics
-
Accelerated cartilage wear and early osteoarthritis
-
Increased risk of total knee replacement decades earlier than expected
The numbers are staggering: approximately 200,000 ACL reconstructions are performed annually in the United States, making this one of the most common knee injuries—especially among active adults aged 15–45.
Traditional ACL Treatment vs. Regenerative Options
When you tear your ACL, you generally have two broad categories of treatment: conventional management and regenerative approaches. Understanding both helps you make an informed decision.
Conservative (Non-Surgical) Care
For some partial tears and sprains, doctors may recommend conservative treatment:
-
RICE protocol (rest, ice, compression, elevation)
-
Anti-inflammatory medications for pain and swelling
-
Knee bracing to provide external stability
-
Physical therapy over 8–12 weeks to strengthen surrounding muscles
This approach works for some patients with minor injuries who don’t need to return to high-demand pivoting sports. However, many people who try conservative care alone continue experiencing instability.
Standard ACL Reconstruction Surgery
ACL surgery involves arthroscopically replacing the torn ligament with a graft. Common graft sources include:
-
Patellar tendon (from your own knee)
-
Hamstring tendons
-
Quadriceps tendon
-
Donor tissue (allograft)
The reconstructive surgery is generally successful, but it comes with significant considerations:
|
Surgical Concerns |
Details |
|---|---|
|
Recovery timeline |
9–18 months of rehabilitation |
|
Return-to-sport rates |
Only 40–60% of athletes return to previous competitive level |
|
Surgical risks |
Infection, bleeding, blood clots, anesthesia complications |
|
Graft complications |
Re-tear, failure, stiffness, persistent pain |
|
Muscle atrophy |
Significant quad weakness during prolonged rehab |
The Regenerative Alternative
Regenerative medicine offers a biological strategy: instead of replacing your ACL with a graft, we help your body repair or reinforce the existing ligament using your own cells.
Bone marrow derived mesenchymal stem cells and platelet rich plasma PRP are the two most-studied biologic options for ligament healing. While clinical evidence continues to evolve, these approaches represent a fundamentally different philosophy—working with your body’s healing process rather than removing and replacing damaged tissue.
ACL Reconstruction and Graft Regeneration: What’s New?
Recent years have brought exciting progress in the field of anterior cruciate ligament (ACL) reconstruction, especially when it comes to improving graft regeneration and long-term ligament healing. Traditionally, ACL reconstruction relied solely on surgical techniques and the body’s natural healing process, but now, regenerative medicine is changing the landscape.
Stem cell therapy—particularly using mesenchymal stem cells (MSCs) derived from bone marrow—has shown promising outcomes in enhancing ACL graft regeneration. These multipotent stem cells can differentiate into ligament fibroblasts and other cell types essential for robust tissue repair. When introduced at the site of ACL reconstruction, stem cells help orchestrate the healing process, supporting the integration and maturation of the new graft.
Combining stem cell injections with platelet rich plasma (PRP) is another innovation gaining traction. PRP is rich in growth factors that stimulate cell proliferation and tissue repair, and when used alongside stem cell therapy, it can further accelerate ligament healing and improve clinical outcomes. Early studies suggest that this combination may reduce recovery time and lower the risk of reinjury after ACL reconstruction.
Researchers are also exploring the best timing and dosage for stem cell injections to maximize their benefits in ACL graft regeneration. While more large-scale clinical trials are needed, the integration of cell therapy into ACL reconstruction protocols is already showing promising outcomes for patients seeking faster, more complete recovery.
How Stem Cell Therapy Works for an ACL Tear
To understand why stem cell injection therapy might help your ACL, let’s look at what these cells actually do.
Stem cells are unique because they can develop into many different types of cells, including those needed to repair damaged ligaments. Stem cells used for ACL therapy are typically harvested from bone marrow, adipose tissue, or donated umbilical cord tissue. After harvesting, the stem cells are processed and injected into the site of the ACL tear to promote healing.
Once introduced to the injury site, stem cells can help reduce inflammation, stimulate tissue regeneration, and support the body’s natural healing processes. During the ligament healing process, cell migration plays a crucial role—stem cells and other cells such as fibroblasts migrate into the graft area, facilitating tissue repair, revascularization, and the formation of new extracellular matrix.
What Are Mesenchymal Stem Cells?
Mesenchymal stem cells are adult stem cells found primarily in your bone marrow and adipose tissue (fat). These multipotent stem cells have two remarkable abilities:
-
They can differentiate into various cell types—including ligament fibroblasts, bone, cartilage, and tendon cells
-
They release powerful growth factors that signal other cells to start repairing damaged tissue
Unlike induced pluripotent stem cell therapies (which are lab-created), bone marrow stem cells and adipose derived stem cells come directly from your own body, minimizing rejection risk.
What Happens After an ACL Tear?
When your ACL tears, several things occur at the cellular level:
-
Disruption of collagen fibers that give the ligament strength
-
Bleeding inside the knee joint
-
Intense inflammation
-
Damage to blood vessels and nerve fibers
-
Formation of fibrous scar tissue (which is weaker than normal ACL tissue)
The ACL’s naturally limited blood supply means the healing process is slow and often incomplete. This is why many complete tears never heal on their own.
How Stem Cell Injections Promote Healing
When we inject concentrated stem cells into and around your injured ACL, several mechanisms activate:
-
Inflammation reduction — Stem cells modulate the immune response, decreasing pain and swelling
-
Collagen production — Growth factors like basic fibroblast growth factor and platelet derived growth factor stimulate cell proliferation and new tissue formation
-
Tendon to bone healing — Cells help reinforce the ACL’s attachment points at the femur and tibia
-
Improved tissue quality — The remodeling and maturation process produces tissue that behaves more like intact ACL than typical scar tissue
At Stem Cells LA, we combine concentrated bone marrow stem cells with platelet rich plasma because PRP provides additional growth factors (PDGF, TGF-β, VEGF) that further stimulate soft tissue repair.
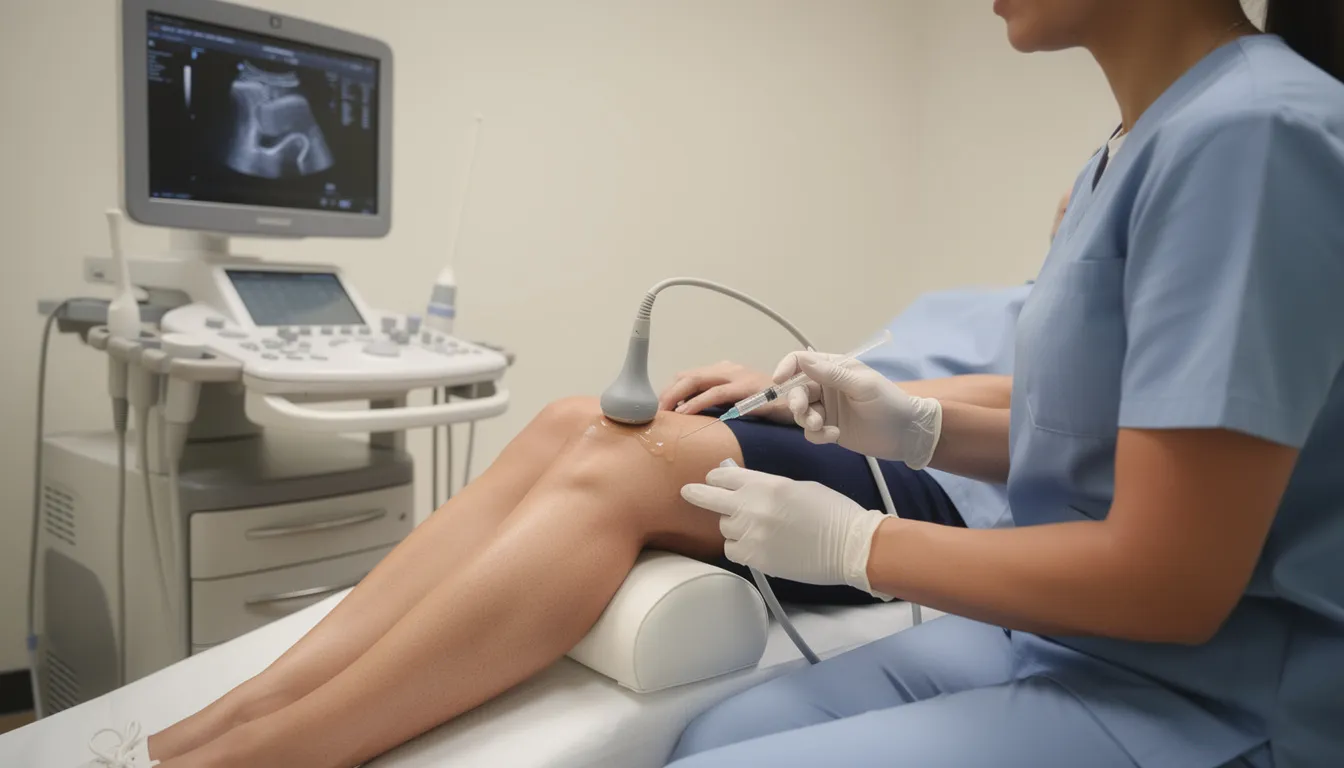
Key advantage: This is a minimally invasive, image-guided injection procedure—not open knee surgery. Most patients walk out the same day and begin guided rehabilitation soon after.
Research supports this approach. Animal studies consistently show improved ACL graft regeneration and ligament healing with stem cell transplantation. Human clinical trials since around 2010 have shown promising outcomes, though results depend heavily on tear type and treatment protocol.
What Types of ACL Tears Respond Best?
Not every ACL tear is a good candidate for stem cell therapy. The best positive outcomes occur with:
Ideal candidates:
-
Partial ACL tears where some collagen fibers remain intact
-
Proximal tears (near the femur) with a preserved synovial covering
-
Acute injuries (typically within 3–6 months) before chronic scarring develops
-
Patients with mild to moderate instability
Less suitable cases:
-
Complete ACL tear with retracted, separated ends
-
Knees that frequently “give way” during normal activities
-
Chronic injuries with extensive fibrous scar tissue formation
For complete mid-substance ruptures, anterior cruciate ligament reconstruction may still be necessary. However, even in these cases, stem cells may serve as an adjunct therapy—supporting post-surgical healing and potentially improving ACL graft regeneration.
How we determine candidacy at Stem Cells LA:
-
Detailed medical history
-
Physical examination (Lachman test, pivot-shift test)
-
Review of MRI imaging
-
Sometimes stress X-rays to quantify laxity
-
Discussion of your goals and activity level
A high-level pivoting athlete may make different choices than a recreational exerciser. We’ll help you understand all options.
Don’t self-diagnose. Send or bring your MRI to our office for physician review during a free consultation.
Bone Marrow and Cell Therapy: A Closer Look
Bone marrow is a powerhouse when it comes to regenerative medicine, serving as a rich source of mesenchymal stem cells (MSCs) that can drive tissue repair and healing. In the context of ACL injuries, bone marrow-derived MSCs have demonstrated the ability to differentiate into ligament fibroblasts and other cell types crucial for ligament healing and reconstruction.
Cell therapy using bone marrow-derived stem cells has shown promising outcomes in both laboratory and clinical settings, helping to restore ligament integrity and function after ACL injuries. These stem cells not only support tissue repair but also modulate inflammation and enhance the overall healing environment within the knee.
Adipose derived stem cells (ADSCs) are also being explored as an alternative to bone marrow-derived MSCs. Harvested from fat tissue, ADSCs offer a less invasive and more accessible cell resource for treating ACL injuries, with early studies indicating similar potential for promoting ligament healing.
Another exciting frontier is the use of induced pluripotent stem cells (iPSCs), which can be programmed to become various cell types, including those needed for ligament repair. While iPSC-based therapies are still largely experimental, they represent a promising direction for future regenerative medicine approaches to ACL reconstruction.
Despite these advances, more research is needed to fully understand how bone marrow and other cell therapies work at the molecular level to support ACL graft regeneration and tissue repair. As clinical trials continue, the hope is that these therapies will offer even better outcomes for patients with ACL injuries.
The Stem Cell ACL Procedure at Stem Cells LA
Understanding exactly what happens during treatment helps many patients feel more comfortable with the process. Here’s a step-by-step overview of what to expect at our Los Angeles/Redondo Beach clinic.
Step 1: Evaluation and Planning
Your journey begins with a thorough consultation. We’ll:
-
Review your MRI and any prior imaging
-
Discuss previous treatments and their outcomes
-
Examine your knee for stability, range of motion, and pain
-
Map the ACL, meniscus, and cartilage status
-
Create a tailored injection plan (some patients benefit from combined ACL + meniscus treatment)
Step 2: Harvesting Your Cells
On procedure day, we collect stem cells from your own body—most commonly from the posterior iliac crest (the back of your pelvic bone).
-
The area is numbed with local anesthesia
-
A specialized needle extracts bone marrow concentrate
-
The procedure takes about 15–20 minutes
-
Discomfort is minimal; most patients describe it as pressure rather than pain
While adipose derived stem cells from fat tissue are sometimes used, bone marrow derived mesenchymal stem cells remain the most studied cell resources for ligament reconstruction and healing. Peripheral blood is also being explored as a source of reprogrammable cells for regenerative therapies.
Step 3: Processing
Your bone marrow is processed on-site using a sterile, closed system:
-
The sample is spun in a centrifuge to concentrate the stem cell fraction
-
We simultaneously draw blood to prepare platelet rich plasma
-
PRP concentrates platelets and growth factors for combination with stem cells
-
Total processing time is approximately 30–45 minutes
Step 4: Image-Guided Injection
This is where precision matters. Using ultrasound and/or fluoroscopy, we:
-
Visualize the injured ACL and surrounding structures
-
Precisely place the stem cell/PRP mixture into the tear site
-
Target the tendon bone interface where the ACL attaches to the femur and tibia
-
Address associated issues (MCL sprains, meniscal fraying, early cartilage thinning) if appropriate
The injection itself takes only a few minutes. You’ll remain awake throughout, with local anesthesia and optional light sedation for comfort.
Step 5: Recovery and Rehabilitation
Post-procedure, we’ll outline a progressive recovery plan:
-
Brief period of reduced weight-bearing or bracing
-
Ice and elevation for the first few days
-
Physical therapy program designed to protect the ligament while stimulating proper tissue repair
-
Gradual progression through strengthening and mobility exercises
Many patients notice pain reduction within weeks. Follow-up MRI at 3–6 months sometimes shows structural improvements in responsive cases.
Safety note: Because we use your own cells (autologous), rejection risk is extremely low. Short-term side effects are typically limited to soreness or swelling at harvest and injection sites.
Timeline: What to Expect After Treatment
Individual results vary, but here’s a general framework:
|
Timeframe |
Typical Progress |
|---|---|
|
Week 1–2 |
Pain control, swelling reduction, knee protection (brace, possible crutches) |
|
Week 3–6 |
Gradual range of motion increase, quadriceps and hamstring activation with PT |
|
Week 6–12 |
Progressive strengthening, low-impact cardio, simple agility work if stability allows |
|
Month 3–9 |
Return to higher-level sports and pivoting activities when functional testing allows |
Important: Overloading the knee too soon can jeopardize ACL healing. We typically reassess clinically at 6–8 weeks and 3–6 months, with repeat MRI in selected patients to document ligament healing progress.

Evidence and Limitations of Stem Cell Therapy for ACL Tears
We believe in transparency. Here’s an honest look at what the science shows—and what we still don’t know.
What Research Tells Us
Preclinical (animal) studies: Since the mid-2000s, numerous animal studies have demonstrated that bone marrow and adipose derived stem cells can:
-
Improve tendon bone healing at graft attachment sites
-
Enhance collagen fiber organization
-
Increase mechanical strength after ACL injury or primary ACL repair
Human clinical research:
-
Small case series using bone marrow concentrate and PRP for partial ACL tears show improved stability and knee function
-
One notable case study documented a 55-year-old tennis player who achieved 80% ACL reattachment on MRI and a Lysholm score of 99/100 (near-perfect function) after three stem cell injections
-
Studies on primary ACL repair with scaffold-seeded stem cells report 90% survival rates at 5-year follow-up
-
Clinical trials for soft tissue injuries continue, with many showing promising outcomes for appropriate candidates
Current Limitations
We must be honest about what stem cell therapy cannot do:
-
Not a guaranteed cure — Success depends on tear pattern, timing, cell quality, injection technique, and rehabilitation commitment
-
Limited large-scale trials — Most human studies are small case series or pilot trials
-
Complete ruptures remain challenging — Many patients with complete ACL tears still need reconstructive surgery
-
Mechanism questions persist — Researchers are still determining whether injected cells directly form new ligament tissue or primarily act through growth factor signaling to enhance the repair environment
At Stem Cells LA, we follow current literature, use evidence-informed protocols, and clearly explain expected benefits, limitations, and alternative treatments before proceeding with any patient.
Risks, Side Effects, and Safety Considerations
Common, mild side effects:
-
Temporary soreness at the bone marrow harvest site (usually 2–5 days)
-
Bruising or swelling around the injected knee
-
Mild inflammatory flare that resolves within a week
Less common risks:
-
Infection (rare with proper sterile technique)
-
Bleeding or hematoma
-
Allergic reaction to local anesthetic
-
No improvement despite treatment
Long-term safety: Because cells are autologous (from your own body), rejection risk is extremely low. Serious complications like tumor formation have not been observed in standard orthopedic applications of adult stem cells, though long-term data continues to accumulate.
At Stem Cells LA, we operate in a medical setting under physician supervision, use strict sterile technique, and carefully screen patients to minimize risk.
Who Is (and Isn’t) a Good Candidate?
Ideal Candidates for Stem Cell ACL Treatment
You may be a good candidate if you have:
-
✅ A confirmed partial tear on MRI, especially proximal tears
-
✅ An acute or subacute injury (typically within 3–6 months)
-
✅ Mild to moderate instability with intact menisci and joint alignment
-
✅ Goals that don’t require maximum pivoting stability (recreational vs. elite athlete)
-
✅ Willingness to commit to a structured physical therapy program
-
✅ Desire to avoid or delay knee surgery
Who May Not Be a Good Candidate
Stem cell therapy may not be right for you if:
-
❌ You have a complete ACL tear with retracted ends and significant laxity
-
❌ You have advanced osteoarthritis or severe cartilage defects
-
❌ You have major meniscal loss requiring separate surgical intervention
-
❌ You’re unable or unwilling to follow post-treatment rehabilitation
-
❌ You’re an elite athlete requiring absolute maximum stability for competitive pivoting sports
Prior surgery doesn’t automatically exclude you. Stem cells and PRP may help with lingering pain, instability, or graft support in select post-reconstruction knees experiencing ongoing issues.
Factors that influence healing potential:
-
Age
-
Activity level and goals
-
General health (smoking and diabetes can impair healing)
-
Body weight
-
Compliance with rehabilitation
Every case deserves individual evaluation. Contact Stem Cells LA to review your MRI and discuss realistic expectations.
Costs, Insurance, and Financing
Let’s address the financial reality:
-
Insurance coverage: Most insurers currently classify stem cell and PRP treatments for knee injuries as elective or investigational and do not cover them
-
Transparent pricing: At Stem Cells LA, we offer flat-rate pricing for ACL-focused procedures, with optional add-ons if additional structures need treatment
-
Financing available: We offer financing options and cash discounts
-
Cost comparison: Total costs are typically significantly lower than the combined expense of ACL surgery, hospital fees, anesthesia, and 9+ months of intensive rehabilitation
Contact our office for an exact quote after your specific case and treatment plan are reviewed.
Next Steps: Schedule Your ACL Stem Cell Consultation
If you’re dealing with an ACL tear, experiencing knee pain, or exploring ways to avoid ACL surgery, we invite you to connect with Stem Cells LA.
We’re located in Los Angeles/Redondo Beach and regularly see patients from across the South Bay, including Torrance, Manhattan Beach, Hermosa Beach, and the greater LA area.
What to Expect at Your Free Consultation
-
Thorough review of your MRI and medical history
-
Physical examination and stability assessment
-
Honest discussion of whether you’re a candidate for stem cell therapy
-
Explanation of alternatives if regenerative treatment isn’t right for you
-
No pressure, no obligation
Consultations can often begin via phone or video for your convenience.
Take Action Now
📞 Call Stem Cells LA directly to schedule your free consultation
📝 Fill out our online form to upload your MRI reports or prior surgical notes
📲 Request a callback to discuss whether stem cell therapy fits your goals and timeline
Time matters. Treating ACL injuries promptly—before chronic scarring and instability develop—maximizes the chance that a biologic, non-surgical approach may be possible. If you’ve recently injured your ACL, don’t wait months to explore your options.

Future Directions for ACL Tear Treatment
The future of ACL tear treatment is rapidly evolving, with a multidisciplinary approach at the forefront. Combining advanced surgical techniques, regenerative medicine, and targeted physical therapy is expected to deliver the best results for patients with ACL injuries.
Stem cell injection therapy is poised to play a major role in enhancing ACL healing and improving clinical outcomes. By harnessing the power of mesenchymal stem cells—whether from bone marrow, adipose tissue, or even synovial fluid—doctors can promote more effective tissue repair and potentially reduce the risk of reinjury.
Innovations in tissue engineering, such as the development of new biomaterials and scaffolds, are also on the horizon. These technologies aim to provide a supportive environment for stem cells, growth factors, and ligament tissue to regenerate more efficiently. Growth factors like basic fibroblast growth factor (bFGF) and platelet derived growth factor (PDGF) are being studied for their ability to accelerate the healing process and improve the quality of repaired ligament tissue.
Clinical trials are underway to determine the safety and efficacy of these regenerative approaches in ACL reconstruction and graft regeneration. As research progresses, we can expect to see more personalized and effective treatment options for ACL injuries, with the goal of restoring knee function, minimizing downtime, and improving long-term outcomes.
Additionally, novel cell therapies—such as synovial mesenchymal stem cells—are being investigated for their unique regenerative properties, offering new hope for treating not only ACL tears but a wide range of sports medicine and soft tissue injuries. As these advances move from the lab to the clinic, the future looks bright for anyone facing an ACL tear.
Key Takeaways
-
Stem cell therapy for ACL tears uses your own mesenchymal stem cells and platelet rich plasma to promote natural ligament healing
-
Best candidates have partial ACL tears, proximal tears, or acute injuries with preserved ligament structure
-
The procedure is minimally invasive, performed in an outpatient setting, with most patients walking out the same day
-
Recovery is typically faster than ACL reconstruction, though individual timelines vary based on injury severity and rehabilitation compliance
-
Clinical evidence is promising but still evolving; stem cell therapy isn’t a guaranteed cure for every ACL injury
-
Complete tears may still require surgical treatment, but stem cells can serve as an adjunct in some cases
Stem cell therapy cannot replace surgery for everyone. But for the right ACL tear at the right time, it may offer a powerful way to reduce pain, restore stability, and get back to the activities you love—with less downtime and without going under the knife.
Contact Stem Cells LA today to find out if you’re a candidate.


